 
Fractures of the proximal humerus occur in typical patterns that are influenced by muscular insertions that cause predictable displacement of each fragment ( Fig. The complex anatomy of the shoulder girdle must be understood in order to successfully treat proximal humerus fractures and shoulder dislocations. The skills of the surgeon and the resources available must also be considered. The goal of treatment is to obtain fracture union and maintain function of the shoulder, while avoiding complications. The management of proximal humeral fractures begins with a thorough assessment of the functional needs and abilities of the patient, the presence of cognitive or physical impairments, the fracture pattern, the bone density, the patient′s expectations, and the ability of the patient to comply with a rehabilitation program. Thus, when treating a proximal humeral fracture, surgeons cannot rely on demonstrated evidence-based guidelines and must use their experience and judgment to decide upon treatment. 15 However, there are no high-quality comparative studies of these new techniques, either to each other or to nonoperative management, to help guide the surgeon. Stabilization of the proximal humerus in polytrauma patients by methods that allow early motion and weight bearing on the injured limb continue to be advocated, and devices such as intramedullary nails and locking plates have been developed that may allow this to be done with less invasive techniques. Whether this is best done by reduction and fixation of the fracture or by prosthetic replacement of the shoulder depends on the patient′s needs and expectations, the fracture pattern, the bone quality, the implants available, and the experience of the surgeon. 14 If a fracture of the proximal humerus is either unacceptably displaced or too unstable to allow early motion, then operative intervention should be considered in any patient who needs or wants to regain useful function of the shoulder. 14 Improved results are seen when active mobilization is allowed before 14 days after injury, compared with delayed mobilization. The importance of early mobilization following even nondisplaced fracture of the proximal humerus has been demonstrated. 
Capsular restriction or loss of these gliding surfaces will render the shoulder stiff and painful and lead to a poor outcome. Shoulder movement depends on the relative gliding of the humeral head, rotator cuff, bursal tissue, and deltoid muscle. 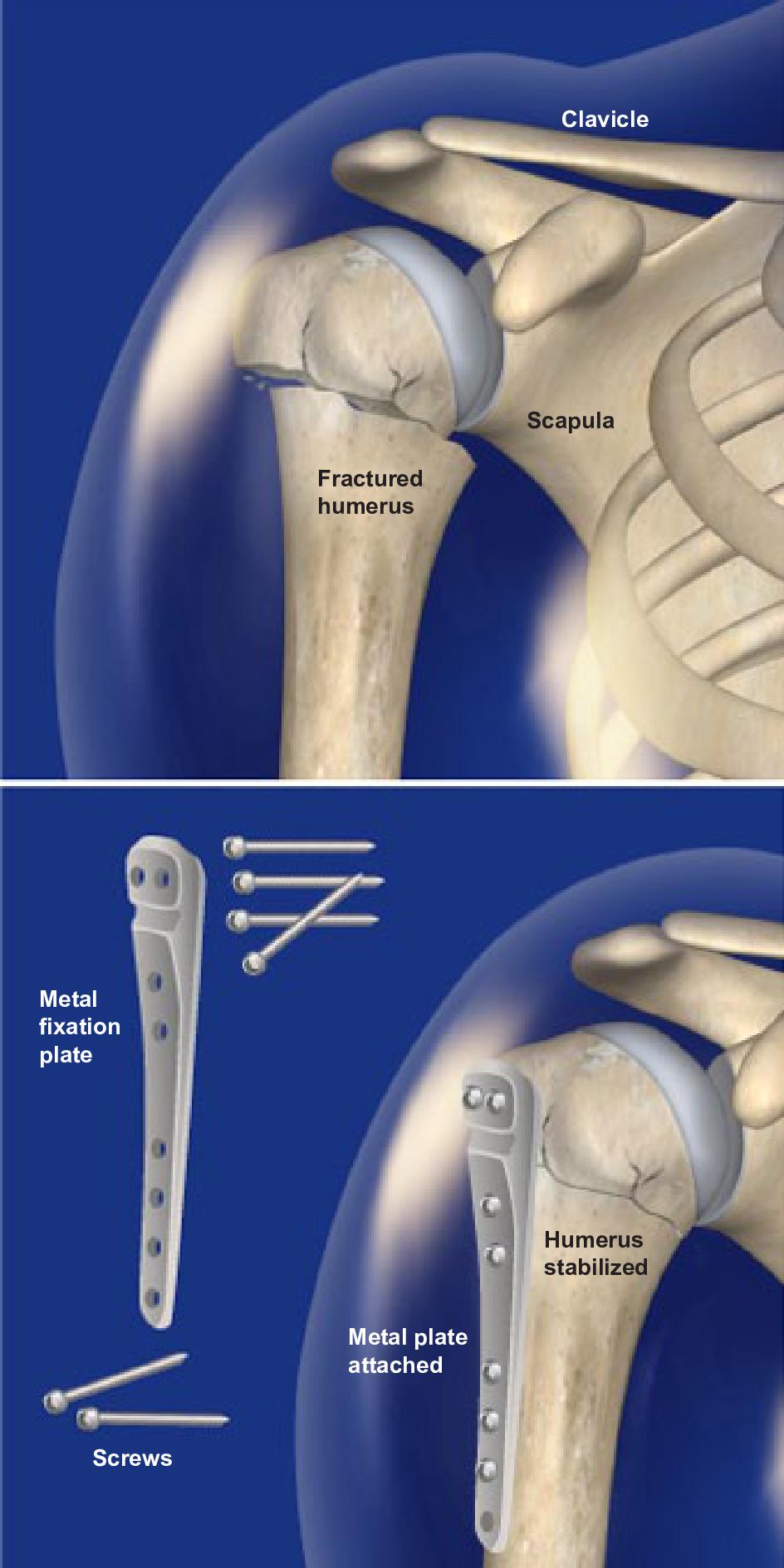
The overriding principle in the treatment of proximal humeral fractures is the need to restore a functional range of motion and to permit the activities of daily living that the specific patient performs. 11, 12 Elderly patients often have an associated injury to the rotator cuff with both fractures and dislocations if present, surgical repair should be considered. Although early surgery is traditionally not considered, arthroscopic evaluation of the recently dislocated shoulder may play a role in defining lesions associated with late instability and may enable early repair, with decreased morbidity from chronic instability. 9, 10 Young patients with traumatic dislocation are those most likely to develop recurrent instability. The natural history of shoulder dislocation with respect to the risk of recurrent dislocation continues to be defined. The goal of treatment is expedient reduction with recovery of full function. 8ĭislocations of the glenohumeral joint are also common and affect persons of all ages. 1– 4 Improved surgical techniques and implants for both reduction and fixation of proximal humeral fractures and for shoulder hemiarthroplasty after fracture have been developed, 5– 7 and outcome studies are now being performed that will help dictate treatment of these diverse injuries. Over the past decade, there has been ongoing controversy about the relative merits of operative versus nonoperative treatment for proximal humeral fractures, as well as uncertainty about whether better results are achieved with internal fixation or hemiarthroplasty. In this circumstance, there is a high incidence of associated injuries, including neurovascular lesions of the injured arm and injuries of the cervical spine and chest. The proximal humerus may also be fractured in younger patients, usually as the result of high-energy trauma. Their incidence is increasing with the aging of the population. Proximal humerus fractures represent up to 5% of all fractures, and they most often occur in an elderly person with osteoporosis as the result of a fall. Proximal Humerus Fractures and Shoulder Dislocations Michael J. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
